What is Heart Dysfunction?
If you have heart failure, you’re not alone. About 1 Crore Indians are living with it today. In fact, it’s one of the most common reasons people age 65 and older go into the hospital. It can take years for heart dysfunction to develop. Heart dysfunction is called congestive heart failure when fluid builds up in various parts of the body. If you haven’t been diagnosed with heart failure but are at risk for it, you should make lifestyle changes now to prevent it! Lifestyle changes may include regular exercise, maintaining a healthy weight, not smoking and controlling blood pressure, cholesterol and blood sugar levels.
Heart dysfunction symptoms usually develop over time as your heart becomes less able to pump the blood that your body needs.

Does Your Heart Stop?
Does your heart stop? When you have heart dysfunction, it doesn’t mean that your heart has stopped beating. It means that your heart isn’t pumping blood as it should. The heart keeps working, but the body’s need for blood and oxygen isn’t being met.
Heart dysfunction can get worse if not treated. It’s very important to understand and follow the treatment plan developed by your health care team. When you make healthy changes, you can feel a lot better and enjoy life much more!
What can happen?
- Your heart does not pump enough blood.
- Blood backs up in your veins.
- Fluid builds up in your body, causing swelling in your feet, ankles, legs and abdomen. This is called “edema.”
- Fluid builds up in your lungs. This is called “pulmonary edema.”
- Your body does not get enough oxygen.
What are the signs?
- Shortness of breath, especially when lying down
- Tired, run-down feeling
- Coughing or wheezing, especially when you exercise or lie down
- Swelling in feet, ankles, legs and abdomen
- Weight gain from fluid buildup
- Confusion or can’t think clearly
What are the causes?
The most common cause of heart dysfunction is coronary artery disease (CAD occurs when arteries that supply blood to the heart muscle become narrowed by buildups of fatty deposits called plaque. This can lead to a heart attack which can damage and weaken the heart muscle and cause heart failure.
Other common causes of heart failure are:
-
- High blood pressure
- Obesity (being overweight)
- Diabetes
- Heart valve disease
- Diseases of the heart muscle (cardiomyopathy)
- Thyroid problems
- Alcohol or drug abuse
- Certain types of chemotherapy
How is it treated?
- Heart failure is treated with several different medications which can reduce symptoms and prolong life.
- A low-sodium (salt) diet can decrease fluid retention.
- If you have coronary or valve disease, stenting or surgery may be necessary.
- Cardiac devices (pacemakers or defibrillators) may be needed.
- In advanced heart failure, heart transplantation may be necessary.
What can I do to manage my heart condition?
Follow the advice of your healthcare team.
-
- If you smoke, quit.
- Take your medicines exactly as prescribed.
- Weigh daily to check for weight gain caused by increased fluid.
- Track your daily fluid intake.
- Monitor your blood pressure daily.
- Maintain a healthy weight to reduce the strain on your heart.
- Avoid or limit alcohol and caffeine.
- Eat a heart-healthy diet that’s low in sodium and fat.
- Eat less salt and salty foods.
- Get regular exercise most days of the week.
- Get adequate rest.
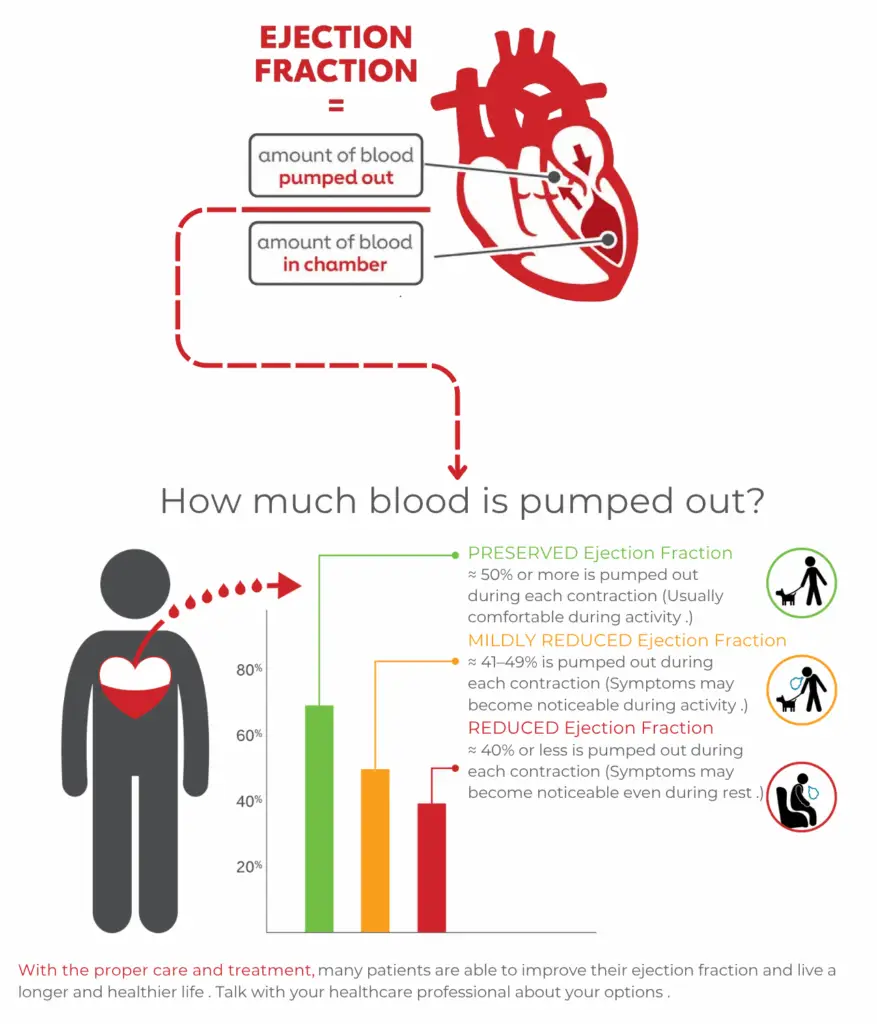
Your Ejection Fraction Explained
The Ejection Fraction compares the amount of blood in the heart to the amount of blood pumped out. The fraction or percentage helps describe how well the heart is pumping blood to the body.
How Can I Live With Heart dysfunction?
About 1 crore Indians are living with heart failure today. In fact, it’s one of the most common reasons why people 65 and older go into the hospital. Fortunately, heart failure can be treated. Getting good medical care, understanding and following the treatment plan developed by your health care team, and learning about heart failure could improve and prolong your life. You can help by taking your medicines as prescribed, and by following your eating and exercise plans.
What medicine might I take?
The goal of treatment is to help you live a longer, better-quality life. Treating the causes of heart dysfunction with medication can lessen tiredness (fatigue), shortness of breath and swelling. It can also help improve your energy level so you can be physically active.
Here are some examples of medicines that may be prescribed:
- Angiotensin Converting Enzyme (ACE) Inhibitor: widens blood vessels, lowers blood pressure, and decreases the heart’s workload.
- Angiotensin Receptor Blocker (ARB): widens blood vessels, lowers blood pressure, and decreases the heart’s workload.
- Angiotensin-Receptor Neprilysin Inhibitor (ARNI): widens the blood vessels, reduces blood pressure, reduces sodium (salt) retention, and decreases the heart’s workload.
- Beta-Blocker: lowers blood pressure, slows heart rate and reduces the heart’s workload.
- Diuretic: helps your body get rid of extra water and sodium.
- Mineralocorticoid receptor antagonist (MRA): a type of diuretic that helps eliminate extra salt and fluid.
- SGLT2 inhibitor: a diabetes medication that can be used to treat heart failure with reduced and preserved ejection fraction.
- Nitrate with hydralazine: two medications that work together to widen blood vessels, lower blood pressure and reduced the heart’s workload.
- Digoxin: helps your heart pump with more force.
What should I watch out for?
Tell your health care team right away if…
- You gain 1.5 Kgs in a day or so.
- You see swelling in your feet, ankles or other parts of your body.
- It’s hard to breathe or your breathing worsens.
- You can’t do what you could do the day before.
- You have “the flu.”
- You get a fever.
- You have chest pain.
Other ways to tell that your heart might not be working the way it should include:
- Coughing up pinkish, blood-tinged mucus.
- Confusion, difficulty thinking, dizziness or lightheadedness.
- Changes in your eating habits or appetite.
- It’s hard to breathe.
What can I do?
- Visit your health care professional and follow your treatment plan.
- Read food labels and avoid foods high in sodium (salt).
- Get regular exercise as recommended by your healthcare team.
Use this checklist to better understand the importance of taking your medication.
- Take medications exactly as prescribed. Follow directions on the bottle carefully.
- Keep a list of all medications you take (including prescription and over-the-counter drugs, vitamins, supplements, and herbal remedies). Bring this list with you to all medical appointments. Also show it to your pharmacist when purchasing over-the-counter remedies. Some can interfere with your prescription medications.
- Refill your medications with plenty of time before they run out.
- Tell your health care team if you have any side effects from the medications.
- Do not stop taking any medications on your own. Talk to your health care team first.
- Talk to your health care team if you have any questions about your medications.
Lifestyle Changes
It is important to make lifestyle changes to manage heart failure. The following information offer some of the top
Quitting Smoking and Using Other Tobacco Products
- Write down the reasons why you quit and look at them. Quitting smoking is one of the most important changes for health and heart failure management.
- Each puff of a cigarette increases heart rate and blood pressure and robs the body of needed oxygen. This is especially harmful if you have heart failure.
- No form of tobacco is safe. This includes e-cigarettes and vaping, cigars, chew, snuff, bidis, and clove cigarettes.
- Quitting takes patience and persistence.
- Making a quit-smoking plan will increase the likelihood of success.
- Using a quit-smoking product makes it much more likely to quit for good.
Restricting Sodium and Alcohol Intake
- Patients with heart failure typically need to restrict sodium intake. Sodium increases fluid retention, which increases blood pressure and puts a greater strain on the heart. It also increases fluid buildup which can lead to swelling in the legs, feet and abdomen, and cause shortness of breath.
- We recommend no more than 1,500 mg of sodium daily for patients with mild heart failure. Patients with more severe heart dysfunction may need to restrict it even further.
- One teaspoon of salt contains 2,300 mg of sodium and sodium is hidden in many foods, especially prepared and fast foods as well as restaurant meals.
- Reaching sodium goals may require you to make significant changes in your eating habits.
- If you have heart dysfunction you should have a conversation with your health care team about whether you can drink alcohol. You might be instructed to abstain from alcohol completely, especially if alcohol intake contributed to your heart failure (alcohol-induced cardiomyopathy).
Staying Active
- Having heart dysfunction does not mean restricting activity. In fact, exercise is essential to help strengthen the heart. It helps increase energy levels and makes the whole body healthier. Studies show that moderate exercise helps decrease the risk of needing hospitalization for worsening heart failure.

How Can I Manage My Weight?
Reaching and maintaining a healthy weight can be a challenge. You may have tried to lose weight before without much long-term success. Be assured, you are not alone. There is no magic weight-loss formula that works for everyone. The key is to find a plan that works for you and provides the right balance of calories and nutrition with the appropriate amounts of physical activity.
What are the keys to healthy weight loss?
To lose weight, you must take in fewer calories than you use through normal metabolism and physical activity. It’s a matter of:
- Watching what you eat.
- Choosing nutritious foods.
- Following an overall healthy diet pattern.
- Getting and staying physically active.
How can I make better food choices?
Follow these guidelines to improve your overall diet pattern.
- Eat a diet rich in fruits, vegetables and whole grains.
- Eat poultry, fish, and nuts and limit red meat.
- Limit how much saturated and trans fats, added sugars, and sodium are in the food you eat.
- Select fat-free and low-fat (1%) dairy products.
- Limit beverages and foods high in calories and low in nutrition.
- Choose and prepare foods with little or no salt.
What happens when I reach a healthy weight?
- After you reach a healthy weight, continue to balance the amounts of calories that you take in with the amount of energy you use each day to maintain your weight.
- After a week, if you’re still losing weight, add a few hundred more calories.
- If you change the amount of physical activity you do, adjust what you eat.
- Keep a record of what you eat and how much physical activity you get so you’ll know how to make adjustments.
How can I stay at a healthy weight?
- Remember that eating smart means eating some foods in smaller amounts and eating high-calorie foods less often.
- Always keep low-calorie, heart-healthy foods around.
- Chopped fruits and vegetables make a great quick snack.
- Use a shopping list, and don’t shop when you’re hungry.
- Plan all your meals. When you’re going to a party or out to eat, decide ahead of time what you can do to make it easier to eat right.
- When you’re hungry between meals or eat a small piece of fruit/nuts.
- When you really crave a high-calorie food, eat a small amount of it. Commit to stay active! Don’t give up on your physical activity plan.